Integrated care has changed.
Not the theory. Not the WHO definition. But the reality.
In England in 2025, integrated care is no longer a patchwork of local pilot schemes, MDT experiments or care-pathway redesign projects. It now lives within a statutory architecture of 42 Integrated Care Systems (ICSs) with legally-mandated duties, population budgets, shared outcomes, and—crucially—Integrated Care Boards (ICBs) under intense financial pressure and severe workforce constraints.
ICSs were created to break down fragmentation, tackle inequalities and improve value. But with ICB running-cost budgets being cut by 50% by October 2025, leadership teams are having to make fewer decisions, faster, with less capacity than ever before.
This change has enormous consequences for MedTech, diagnostics, digital health, biotech, and pharma innovators, and equally for ICS and NHS leadership teams trying to assess and adopt genuine innovation amidst resource constraints.
This article explains:
- What ICSs actually are in 2025
- How reimbursement works now (and where the real levers are)
- How MedTech/IVD/digital/pharma should approach ICSs under the new model
- What ICS/ICB leaders want from suppliers
- How investors should interpret the ICS environment
This is the version of “integrated care” you now need to understand.
1. What ICSs Actually Are in 2025
England is still organised into 42 Integrated Care Systems, each covering between 500,000 and 3 million people.
Official ICS overview:
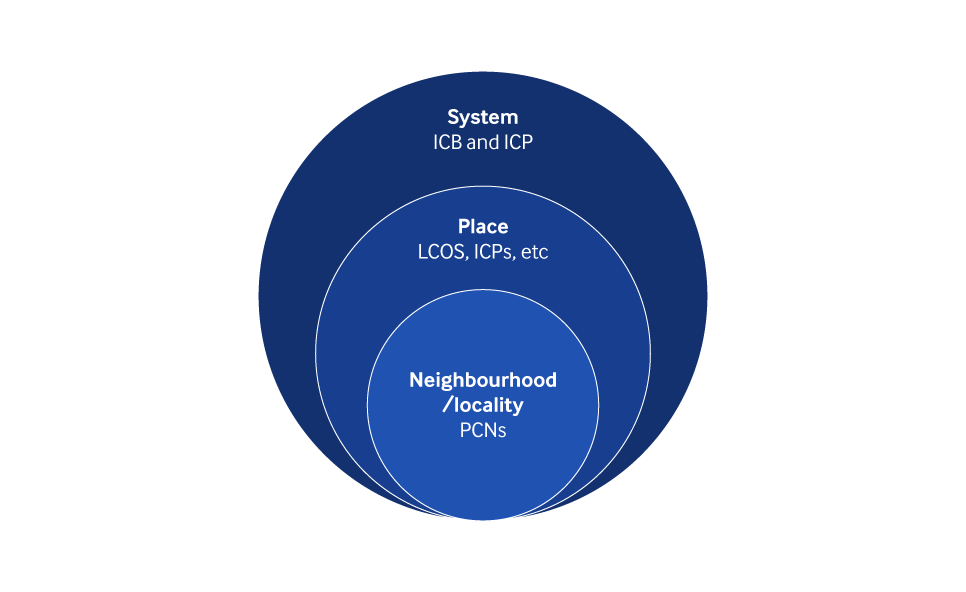
Every ICS has two statutory components:
1. Integrated Care Board (ICB) – The NHS Statutory Body
- Holds the majority of NHS revenue for the area
- Sets commissioning strategy
- Leads population health, finance, elective recovery, urgent care, cancer, CVD, mental health and primary care oversight
- Now shifting to “strategic commissioning only” due to mandated 50% running-cost cuts
2. Integrated Care Partnership (ICP) – The Broader Local Alliance
- Includes local authorities, VCSE, social care, police, universities
- Sets the Integrated Care Strategy
ICS statutory purposes (from the ICS Design Framework):
- Improve outcomes
- Reduce inequalities
- Enhance productivity and value
- Support social & economic development
From 2025 onward, ICBs must deliver these functions with half the management capacity, pushing systems into a new phase: ICSs as lean, strategic purchasers, not large programme-delivery organisations.
For suppliers, this changes everything.
2. Reimbursement in the ICS Era: The Real Levers

You do not win in 2025 by pitching “cost-saving technology”. Everyone says that.
You win by showing:
- Where your product sits within the NHS Payment Scheme
- Which budget holder pays for it
- How the ICS recovers savings
- How it fits population-health and inequality duties
- How it integrates digitally under DSIC
These are the real levers:
2.1 NHS Payment Scheme (NHSPS)
The NHS Payment Scheme is the successor to the National Tariff and sets the rules for how providers are paid.
Overview:
Under NHSPS 2024/25 and 2025/26, the dominant mechanisms are:
- Blended payments (e.g., urgent care, elective care, maternity)
- Aligned incentive contracts (providers share risk/outcomes)
- Local prices for innovative care models
- High-cost device or drug reimbursement arrangements
If your technology does not clearly show how it fits these mechanisms, you are giving the ICS finance team extra work — at a time when half their analysts may soon be gone.
2.2 Who Pays?
The “Who Pays?” guidance determines which ICB is financially responsible for a given patient/service.
Guidance:
You must identify:
- Whether your pathway is ICB-funded, specialised commissioning, delegated specialised, or regional collaborative
- Whether use is tied to patient residence or provider location
- Whether it fits core ICB budget, primary care delegated budget, or system transformation funds
This tells you which budget holder owns adoption.
2.3 High-Cost Drugs & Devices, and Prior Approval
Many innovations are funded as:
- High-cost devices (outside blended payments)
- High-cost drugs (with strict indication criteria)
- Diagnostics requiring prior approval
ICBs often create system-wide formularies, meaning one approval unlocks access across multiple providers.
This is a critical entry-point for IVDs and MedTech.
2.4 Specialised Commissioning Delegation
Almost all specialised services (e.g., cancer, renal, ICU, genomics, transplants, major cardio) are being delegated to ICSs or ICS collaboratives by 2026.
Details:
Result:
If your diagnostic or therapy supports a specialised pathway, the real buyer may no longer be NHS England — it may be the ICS or a regional collaborative.
This is where many oncology, cardiology, AI-diagnostic and advanced therapeutics companies win or lose.
2.5 MedTech Funding Mandate (MTFM)
For technologies that are cost-saving within 3 years, NHS organisations are required to adopt them.
MTFM guidance:
If you meet the criteria, ICS adoption bypasses many of the usual local barriers.
2.6 Digital Reimbursement & DSIC
Digital Services for Integrated Care (DSIC) sets the digital standards ICSs must meet.
Overview: https://digital.nhs.uk/services/digital-services-for-integrated-care
If your technology cannot integrate with:
- ICS shared care records
- NHS App APIs
- FHIR messaging
- Population health management platforms
…you will not pass ICS digital assurance.
Digital health companies must speak architecture, not “dashboards”.
3. The “Thin ICB Era”: What ICS Leaders Want in 2025

Because running-cost budgets will be halved, ICS leaders want:
1. Fewer, bigger decisions
You must show alignment with the ICS Joint Forward Plan, not a single trust’s problem.
2. Pathway-level value
ICBs do not buy products — they buy changes in pathway economics.
3. Solutions with low implementation burden
You must arrive with ready-made:
- Implementation plans
- Data templates (aligned to PLICS & NHSPS)
- Evaluation frameworks
- Digital integration packs
4. Population health and inequalities impact
ICBs are legally obligated to tackle inequalities — your case must reflect this.
5. Ability to scale across the ICS
ICBs want technologies able to spread across:
- Community
- Acute
- Primary care
- Virtual wards
- Neighbourhood teams
6. Alignment with workforce pressures
If you increase staffing requirements, you are dead on arrival.
4. The ICS Access Strategy: A Practical, Step-By-Step Framework
This is the high-performing blueprint used by companies who actually secure ICS-level adoption.
Step 1 — Target the Right ICSs (Evidence + Demographics + Pathway Fit)
Do not blanket-email 42 systems.
Assess:
- Disease burden
- Waiting-time pressure
- Inequality metrics
- Cancer/Emergency/Elective performance
- Digital maturity
- Local clinical champions
Step 2 — Start With Their Strategy, Not Your Product
Download each ICB’s:
- Integrated Care Strategy
- Joint Forward Plan
- Operational Plan
These are public documents on each ICB website.
Create a one-page mapping:
- ICS priority → your intervention
- ICS inequality target → your population segment
- ICS workforce gap → your productivity impact
- ICS digital programme → your integration approach
- ICS financial challenge → your pathway savings
Step 3 — Build the NHS Payment Scheme Case (This Is Where Most Companies Fail)

For your intervention:
- Map the current pathway
- Map the proposed pathway
- Identify which costs are under:
- Blended payment
- Aligned incentive
- High-cost list
- Specialist commissioning
- Primary care delegated budgets
- Model the system-level financial impact, not just provider-level
Arrive with a draft price, not a vague statement.
Step 4 — Do the “Who Pays?” Work
State clearly:
- Which ICB pays
- Under which responsibility rule
- Whether cross-border care applies
- Whether specialised commissioning is moving to ICS level
If you do not do this, the ICB will not do it for you.
Step 5 — Build Your Digital & Data Integration Pack
Include:
- ICS Shared Care Record integration
- FHIR endpoints
- Population health management compatibility
- Federated Data Platform alignment (if relevant)
- IG pack aligned to NHS DSPT
- Cyber Essentials Plus roadmap
This is non-negotiable.
Step 6 — Create a “Thin-ICB” Implementation Model
ICBs no longer have programme managers to spare.
Bring:
- A host provider
- A local clinical champion
- A two-site pilot
- A predefined evaluation methodology
- A scale-up plan requiring minimal ICB capacity
Position yourself as a low-burden, high-impact solution.
Step 7 — Align to Regional & System Influencers
Because ICBs are being shrunk, regional bodies gain power:
- Regional NHSE medical directors
- Regional digital teams
- Specialised commissioning oversight groups
- Clinical networks (cancer, CVD, diagnostics, maternity)
- Health Innovation Networks
- GIRFT national clinical leads
Securing one of these can unlock multiple ICSs.
Step 8 — Present the “Whole System Value” Case
Investors, ICS execs and clinical leaders respond to:
- Reduced avoidable admissions
- Better early diagnosis
- Reduced time to treatment
- Lower unwarranted variation
- Workforce productivity
- Fewer delayed transfers of care
- Better outcomes in high-deprivation populations
This is the language of ICSs in 2025.
5. What Success Looks Like in 2025–2027

Technologies that succeed under ICS 2.0 share these traits:
- A clear inequality impact
- A provable workforce benefit
- Pathway-level economics compatible with NHSPS
- Simple digital integration
- A host provider ready to run programmes
- Minimal ICB overhead
- A system-wide narrative
- Clinically unavoidable — not optional
- Cross-ICS scalability
This is the new bar.
6. What Investors Should Know

The ICS environment is harsh — but clarity is increasing:
For investors:
- Technologies with strong pathway economics will scale faster
- ICS consolidation (likely fewer, larger systems) will create more predictable procurement
- Digital companies must prove real interoperability, not pilots
- Diagnostics with trust-level evidence but no ICS-level economic model will stall
- The winners are companies built for system-level value, not site-by-site sales
ICSs may be under strain, but the market for innovation is not shrinking — it is consolidating into a system-level adoption model.
7. Final Thoughts
Integrated Care Systems have become the central gateway for bringing new technologies into the NHS. Success in 2025 depends on proving real value: stronger outcomes, lower costs, faster diagnosis, reduced waiting times and improved workforce capacity. MedTech, diagnostics, digital health and pharma companies that align to the NHS Payment Scheme, commissioner responsibility rules and digital standards will move faster through the system — and scale more rapidly.
The NHS is changing, and the adoption model is changing with it. The organisations that understand how to work with ICSs, speak the language of population-health value, and bring ready-to-deploy, low-burden solutions will be the ones that thrive.
For MedTech, diagnostics, digital health, pharma and biotech, the message is direct: bring clear evidence, deliver measurable pathway impact, align to system priorities, and make adoption effortless. Companies that do this will scale. Those that don’t will be left behind. The next three years will determine which technologies become part of the NHS operating model — and which never move beyond a pilot.
ICSs were designed to integrate care.
The ICB cuts have forced them to prioritise with a scalpel.
This new environment rewards:
- Strong evidence
- Clear economics
- Digital integration
- Low implementation burden
- Population-level value
- Strategic alignment
For MedTech, diagnostics, digital health, biotech and pharma, the message is clear:
If you can speak the language of pathways, payment mechanisms, population health and productivity — ICSs will listen.
If you cannot, the system will move on without you.
References
NHS England – Integrated Care Systems (Official Overview)
https://www.england.nhs.uk/integratedcare/what-is-integrated-care/
Explains what ICSs are, how they are structured, their statutory roles, and the formal responsibilities of ICBs.
NHS England – NHS Payment Scheme (2025/26)
https://www.england.nhs.uk/pay-syst/nhs-payment-scheme/
The official national rules on how NHS providers are paid, including blended payments and aligned incentive models.
NHS England – “Who Pays?” Commissioner Responsibility Guidance
https://www.england.nhs.uk/publication/who-pays-determining-which-nhs-commissioner-is-responsible-for-commissioning-healthcare-services-and-making-payments-to-providers/
Defines which ICB must fund a service or patient pathway. Essential for mapping payer responsibility.
NHS England – Specialised Commissioning (Delegation & Transformation)
https://www.england.nhs.uk/commissioning/spec-services/
Describes which services are specialised, how they are funded, and how responsibilities are being transferred to ICS collaboratives.
Digital Services for Integrated Care (DSIC) – NHS Digital
https://digital.nhs.uk/services/digital-services-for-integrated-care
Sets standards for interoperability, shared care records, data flows and digital assurance across ICSs.
NHS Shared Care Records Programme
https://digital.nhs.uk/services/shared-care-records
The technical and governance framework for ICS-wide shared care records.
NHS Procurement & Commercial Hub (Digital Primary Care)
https://www.england.nhs.uk/digitaltechnology/digital-primary-care/commercial-procurement-hub/
Practical guidance on procurement routes, commercial models and approval requirements for digital and MedTech suppliers.
NHS Confederation – State of Integrated Care Systems 2024/25
https://www.nhsconfed.org/publications/state-integrated-care-systems-202425
Independent analysis of ICS performance, pressures, governance, and strategic maturity.
2025/26 NHS Priorities and Operational Planning Guidance
https://www.nhsconfed.org/publications/202526-nhs-priorities-and-operational-planning-guidance-what-you-need-know
Summarises national ICS priorities (elective recovery, urgent care, diagnostics, mental health, etc.)
King’s Fund – Integrated Care Systems Explained
https://www.kingsfund.org.uk/insight-and-analysis/long-reads/integrated-care-systems-explained
Neutral, authoritative overview of ICSs — their purpose, statutory duties, governance and challenges.
King’s Fund – ICB Cuts: What Does It Mean?
https://www.kingsfund.org.uk/insight-and-analysis/blogs/icb-cuts-what-does-it-mean
Analysis of the 50% ICB running-cost reduction and the implications for commissioning, system leadership and workforce capacity.
Government of the UK – 10-Year Health Plan for England
https://www.gov.uk/government/publications/10-year-health-plan-for-england-fit-for-the-future
Sets out national strategy for prevention, digital transformation, and community-based care; frames ICS long-term direction.
National Casemix Office – HRG Grouper Tools (Casemix)
https://digital.nhs.uk/services/national-casemix-office/downloads-groupers-and-tools
Provides grouper tools used for NHS Payment Scheme modelling, pathway costing and economic evaluation.